We harness promising vector technology for EID vaccine development
The DDL develops EID vaccines that are based on the vesicular stomatitis virus (VSV) vector. DDL scientists specialize in the same VSV vector that is used in ERVEBO®, Merck’s single-dose Ebola Zaire virus vaccine, which has been used extensively in adults and children. Hundreds of thousands of people in West Africa have received this safe, effective vaccine, which is now licensed in more than a dozen countries.
If proven effective, we’re hopeful that vaccine candidates built on VSV will be similarly important for future EID outbreak responses. Watch our video below on how VSV vaccines work.
EID pathogens we prioritize

More about what we do at the DDL
- Develop new viral vectors and immunogens
- Test vaccine concepts in vivo
- Develop laboratory tests to characterize vaccine candidates and the immune responses they induce
- Educate students and local communities about vaccine science
- Collaborate with other scientists
- Publish research in scientific journals
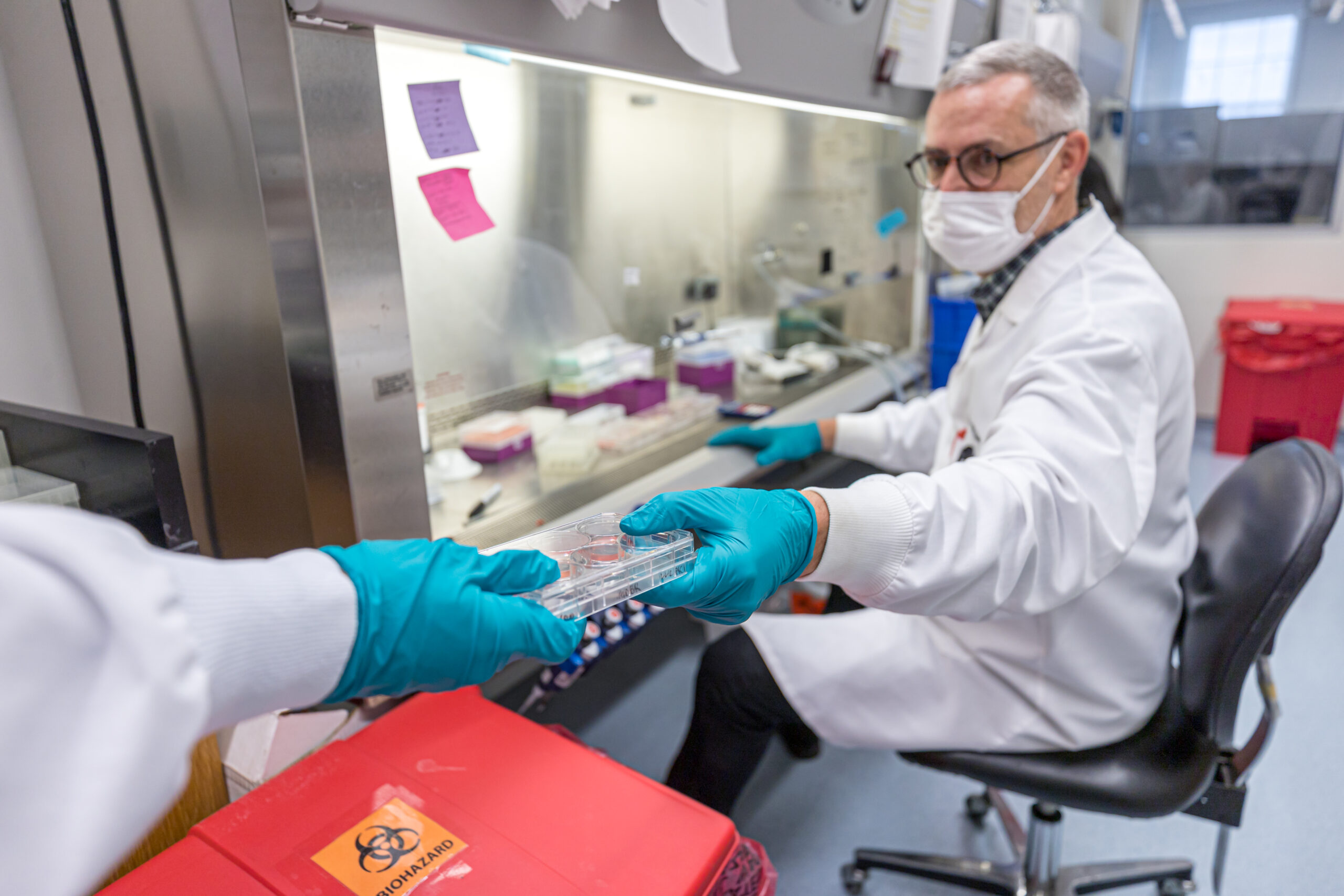
Our global network of collaborators & supporters
The DDL collaborates with investigators at the following institutions, among others:
- IAVI Neutralizing Antibody Center
- Seattle Children’s Research Institute
- Ragon Institute of Massachusetts General Hospital, MIT and Harvard
- University of Texas Medical Branch
- Boston University’s National Emerging Infectious Diseases Laboratories
- University of North Carolina
- Scripps Research Institute
- La Jolla Institute for Immunology
Work at the DDL is supported by
- Coalition for Epidemic Preparedness Innovations
- Government of Japan
- U.S. Biomedical Advanced Research and Development Authority
- U.S. Defense Threat Reduction Agency
- U.S. National Institutes of Health (NIH)
- U.S. NIH National Institute of Allergy and Infectious Diseases
Read selected publications by DDL investigators and their collaborators
Nonhuman Primates Are Protected against Marburg Virus Disease by Vaccination with a Vesicular Stomatitis Virus Vector-Based Vaccine Prepared under Conditions to Allow Advancement to Human Clinical Trials Vaccines (Basel). 2022;10(10). Epub 2022/10/28. DOI: 10.3390/vaccines10101582. (Open access).
An introduction to the Marburg virus vaccine consortium, MARVAC PLoS Pathog. 2022;18(10):e1010805. Epub 2022/10/14. DOI: 10.1371/journal.ppat.1010805. (Open access)
Preclinical immunogenicity and efficacy of a candidate COVID-19 vaccine based on a vesicular stomatitis virus-SARS-CoV-2 chimera EBioMedicine. 2022;82:104203. Epub 2022/08/02. DOI: 10.1016/j.ebiom.2022.104203. (Open access)
Non-neutralizing Antibodies May Contribute to Suppression of SIVmac239 Viremia in Indian Rhesus Macaques. Front Immunol. 2021; 12: 657424. (Open access)
Rectal Acquisition of Simian Immunodeficiency Virus (SIV) SIVmac239 Infection despite Vaccine-Induced Immune Responses against the Entire SIV Proteome. J Virol. 2020 Dec; 94(24): e00979-20. (Open access)
The Frequency of Vaccine-Induced T-Cell Responses Does Not Predict the Rate of Acquisition after Repeated Intrarectal SIVmac239 Challenges in Mamu-B*08(+) Rhesus Macaques. J Virol 93(5). DOI: 10.1128/JVI.01626-18. 2019. (Open access)
Bacterially expressed HIV-1 gp120 outer-domain fragment immunogens with improved stability and affinity for CD4-binding site neutralizing antibodies. J Biol Chem 293(39): 15002-15020. DOI: 10.1074/jbc.RA118.005006. 2018. (Open access)
Mamu-B*17(+) Rhesus Macaques Vaccinated with env, vif, and nef Manifest Early Control of SIVmac239 Replication. J Virol 92(16). DOI: 10.1128/JVI.00690-18. 2018. (Open access)
First-in-Human Evaluation of the Safety and Immunogenicity of an Intranasally Administered Replication-Competent Sendai Virus-Vectored HIV Type 1 Gag Vaccine: Induction of Potent T-Cell or Antibody Responses in Prime-Boost Regimens. J Infect Dis 215(1): 95-104. DOI: 10.1093/infdis/jiw500. 2017. (Open access)
Canine distemper virus neutralization activity is low in human serum and it is sensitive to an amino acid substitution in the hemagglutinin protein. Virology 482: 218-224. DOI: 10.1016/j.virol.2015.03.035. 2016. (Open access)
Vaccine-Induced Simian Immunodeficiency Virus-Specific CD8+ T-Cell Responses Focused on a Single Nef Epitope Select for Escape Variants Shortly after Infection. J Virol 89(21): 10802-10820. DOI: 10.1128/JVI.01440-15. 2015. (Open access)
